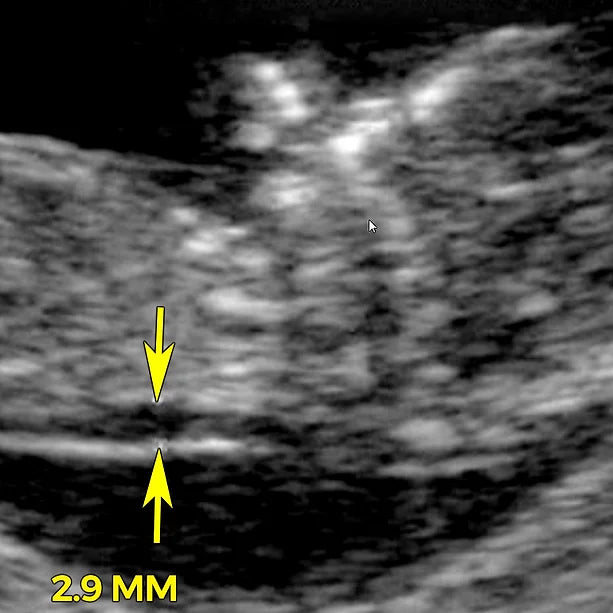
Nuchal translucency (NT) is a collection of fluid under the skin at the back of your baby's neck. The amount of fluid is measured during an NT ultrasound scan:
- between 11 weeks and 13 weeks plus six days of pregnancy
- or when your baby measures between 45mm and 84mm, crown to rump
All developing babies have some fluid at the back of their neck. But many babies with Down syndrome or other chromosomal conditions have an increased amount. That’s why the NT scan is used to help screen for Down syndrome.
Why might I have a nuchal translucency scan?
All pregnant women in Australia are offered an NT scan, to help assess whether or not their babies are likely to have Down syndrome. Every woman has a chance of giving birth to a baby with Down syndrome, & the chance increases the older you get. A screening test tries to get a clearer estimation of how likely it is that your baby has Down syndrome but can't tell you for sure. For example, if the result of your scan shows that you have a one in 1,000 chance, this means that for every 1,000 babies with your level of likelihood, one will have Down syndrome. A chance of more than one in 300 is generally considered high, because it means that for every 300 babies with your level of likelihood, one will have Down syndrome. Diagnostic tests, such as chorionic villus sampling (CVS) and amniocentesis, can say for sure whether or not your baby has Down syndrome or another chromosomal condition. The screening test combines the NT scan result, with a blood test and other factors, such as your age. The test is designed to give you as much information as possible, so you can decide whether or not to go ahead with a diagnostic test.
Do I have to have an NT scan?
It is your choice whether to have one, but even if you don't want your baby screened for Down syndrome, it's still a good idea to have the scan. During the scan, the sonographer will also check the overall health of your baby.
How is the nuchal translucency scan performed?
An NT ultrasound scan must take place between 11 weeks and 13 weeks plus six days, or when your baby’s crown rump length (CRL, the length from his head to bottom) is between 45mm and 84mm. It’s difficult to do the scan before 11 weeks because your baby is still so small. It’s too late to do the NT scan after 14 weeks, because any excess nuchal fluid may be absorbed by your baby's developing lymphatic system. The scan is usually done through your belly using normal ultrasound equipment. It shouldn't hurt, though you may feel some pressure as the sonographer presses the transducer into your skin to get a good view.
How accurate is the nuchal translucency scan?
The NT scan on its own picks up about 77 per cent of babies with Down syndrome. Sometimes, though, a scan can suggest that a baby has a high chance of having Down syndrome, even though the likelihood is actually low. This is called a false positive. The false-positive rate for an NT scan is five per cent. This means that one woman in 20 is wrongly given a high-chance calculation based just on her NT scan results. But the NT scan is rarely done alone. Combining an NT scan with a blood test gives a more accurate result. The blood test measures the levels of the hormone free beta-hCG and the protein PAPP-A. Babies with Down syndrome tend to have high levels of hCG and low levels of PAPP-A. When the NT scan is combined with this blood test, the detection rate increases to 90 per cent. This is called the combined test. The combined test also takes into account factors such as your age and ethnicity, and whether you have diabetes or have ever had a child with Down syndrome. These factors all affect the likelihood that your current baby has a chromosomal condition. Some ultrasound providers may also add other ultrasound findings to the calculations, such as whether they can see a nasal bone, or certain blood flow changes within your baby's heart. The most accurate screening test is a non-invasive prenatal test (NIPT), which is only available privately. It has a detection rate of 99 per cent. NIPT has a false-positive rate of 0.1 per cent, which means it gives fewer false-positive results than the combined test.
What if I have a high chance of Down syndrome?
Most women given a high chance (generally higher than one in 300) will go on to have a baby without Down syndrome. Even with a chance as high as one in five, there's a four out of five chance that your baby doesn't have Down syndrome. If you fall into the high-chance category, your caregiver may refer you to a specialist doctor or a genetic counsellor. During pregnancy, the only way to know for certain that your baby has Down syndrome or another chromosomal abnormality, is to have a diagnostic test, such as CVS or amniocentesis. As these tests carry a small risk of miscarriage, this decision can be difficult, but you don't have to decide in a hurry. One advantage of the combined test is that you have it early in your pregnancy, which gives you time to decide your next steps. It's possible to have a CVS and get the result while you're still in your first trimester. If you're unsure, you can wait until 15 weeks and have an amniocentesis. If you’re given a high-chance result from your combined test, your doctor or midwife may suggest doing a non-invasive prenatal testing (NIPT). NIPT is a more accurate screening test than the combined test, and if your result shows a low likelihood of Down syndrome, it's very unlikely your baby has the condition. So you may only need to consider a CVS or amniocentesis if the NIPT result confirms that your baby has a very high chance of a chromosomal abnormality. NIPT is currently only available privately. Some parents who discover that their unborn baby is affected by abnormalities may consider the difficult decision about whether to end the pregnancy. But you should never be expected to consider ending your pregnancy based on NT scan findings alone. Always ask for a second opinion if you’re in any way unhappy with the advice you're given.
Source: https://www.babycenter.com.au/a544491/nuchal-translucency-nt-scan